Voice AI for Insurance: Renewals, Claims & Policy Queries Without Agent Load
source on Google

It begins before office hours. A policyholder's term plan expires in 11 days. An automated notification has gone out - but into a queue of 40,000 others. Three human agents are scheduled to handle outbound renewals today. By 6 PM, 34% of those callbacks remain untouched. By the time the next cycle runs, some of those policyholders lapse without being reached.
It is the structural reality of insurance contact centers across India. The country processes hundreds of millions of policy renewals, claim inquiries, and customer service calls every year. The vast majority land on human-staffed floors that are chronically under-resourced. Premium reminder calls go unanswered. Claim status queries sit in queues measured in hours.
Renewal drop-off rates compound each quarter, eroding margins that are already under pressure from rising acquisition costs.
The tools to resolve all three - intelligently, at scale, without ballooning headcount - exist today. Voice AI agent has matured from a novelty to a production-grade infrastructure layer that handles millions of insurance interactions with the personalization, compliance architecture, and integration depth that the sector demands.
This blog makes the case for why 2026 is the year enterprises make voice AI for insurance the centerpiece of their CX transformation - and what separates a vendor worth deploying.
ALSO READ: Voice Agents for BFSI: High-Compliance Conversations at Enterprise Scale
The Insurance Contact Center's Structural Problem
Volume without end: Why insurance calls never plateau
Insurance contact centers do not have seasonal peaks in the conventional sense - they have seasonal floors.
Every month brings a fresh cohort of renewal reminders, a new batch of claim status inquiries, and a continuous stream of policy queries from a policyholder base that spans urban professionals to first-time rural buyers.
The call types are entirely predictable:
- Premium renewal reminders
- Lapse recovery outreach
- Claim status updates
- KYC completion nudges
- Surrender query handling
- New policy welcome calls
- Coverage explanation requests
What is not predictable is the sheer volume at which they arrive simultaneously. A mid-size general insurer processing 500,000 active policies may need to execute 200,000 outbound reminder calls in a single renewal fortnight - a figure no human workforce can absorb without severe degradation in contact rates and conversion.
Headcount-based scaling is structurally broken in insurance because the economics do not close. Hiring, training, and retaining agents for work that is inherently repetitive and rule-driven generates turnover rates that erase efficiency gains.
Meanwhile, the underlying volume problem does not diminish - it compounds as policy books grow. The only viable path forward is intelligent automation that handles the predictable, high-volume interactions so that human agents can focus on the cases that genuinely require judgment and empathy.
The high cost of unanswered renewal calls
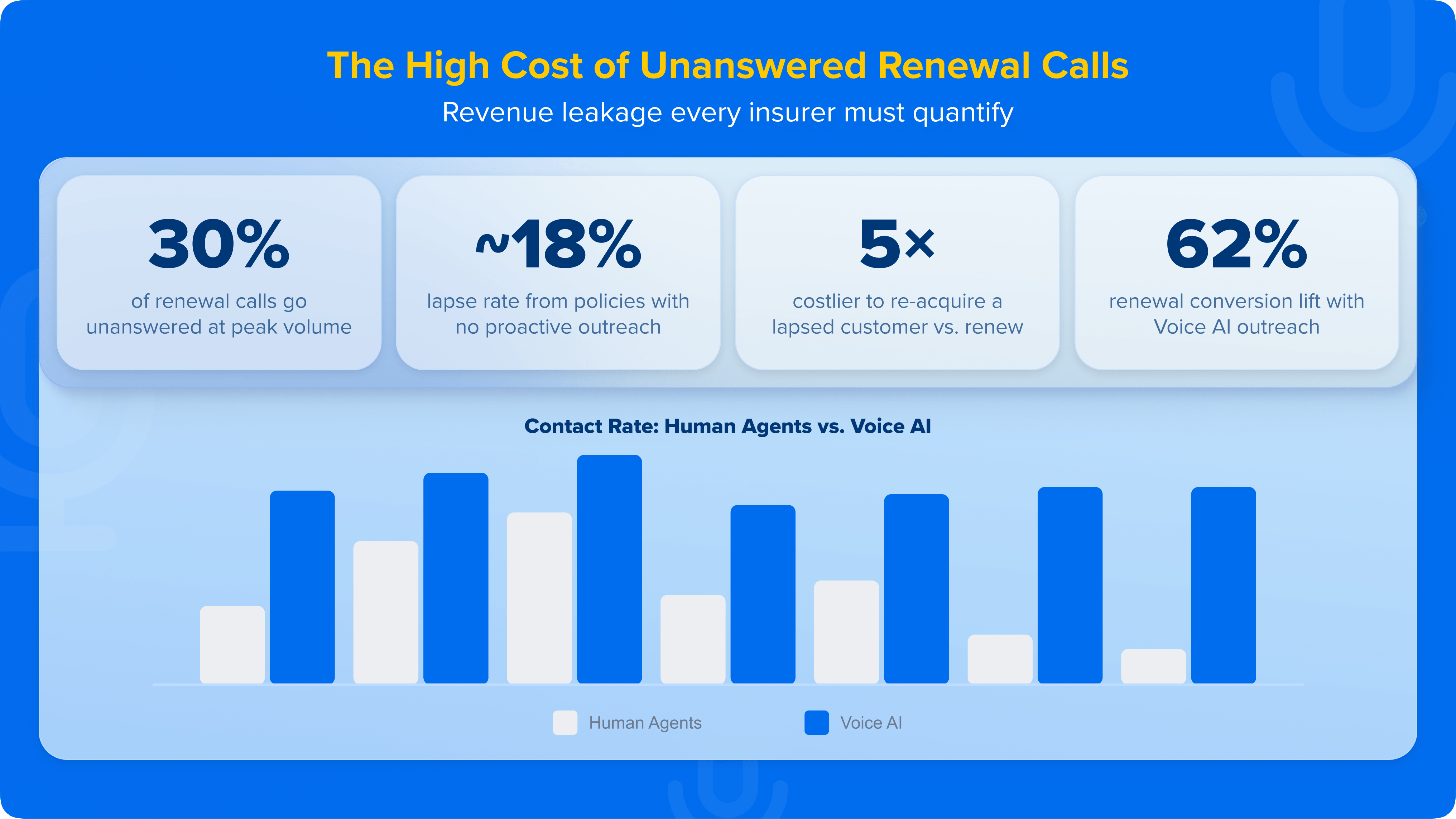
A single missed renewal call is a revenue event.
For a term policy with an annual premium of Rs. 45,000, a lapse triggered by non-contact translates directly to lost premium income, potential surrender payouts, and the significantly higher cost of re-acquisition if the customer can be recovered at all.
Research shows that re-acquiring a lapsed policyholder can cost companies 5x or more compared to retaining them through proactive outreach.
ALSO READ: Scaling Voice AI for Large Enterprises: What Changes After 10 Million Calls
At scale, the numbers get consequential quickly. Insurers with books of 1 million policies or more are, in aggregate, leaving crores in premium revenue on the table each renewal cycle because no voice reached the customer in time.
IRDAI Guidelines and the Compliance Pressure on Every Interaction
Voice interactions in insurance are regulated.
IRDAI's guidelines on fair practice codes, policyholder protection, and telemarketing conduct impose specific obligations on every outbound and inbound call an insurer makes. These include mandatory disclosure language before any product discussion, explicit consent capture for data usage and communication, strict adherence to DND registry checks before outbound dialing, and comprehensive call recording and audit trail requirements for grievance redressal.
RELATED: Data Privacy in Voice AI: The Enterprise Compliance Guide for 2026
For insurers building voice AI infrastructure, compliance cannot be an afterthought - it must be baked into the conversation architecture. This means pre-scripted disclosure flows that activate at the correct point in the interaction, dynamic DND list validation before each dial, consent acknowledgment capture as a structured data event rather than a verbal assertion, and interaction logs that are query-able for regulatory review.
Haptik's voice AI platform is designed with this compliance layer as a first-class component, not a bolt-on feature.
Core Voice AI Use Cases for the Insurance Value Chain
Premium renewal reminders
The renewal reminder call is the most financially consequential interaction in the insurance cycle - and the one that’s often poorly executed.
Generic reminder calls that recite policy numbers and due dates convert at low rates because they feel transactional. Policyholders tune them out.
Intelligent outbound voice AI changes this by personalizing the renewal conversation in real time. Before the call is placed, the system pulls policy type, expiry date, premium history, and customer interaction history from the policy administration system.
The conversation is then constructed around the specific policy - referencing the sum assured, the upcoming due date, and in some configurations, the customer's prior interaction preferences (preferred call time, language, escalation history).
READ: Voice Agents for Enterprises: How Inbound and Outbound Calling Works?
Haptik's outbound voice AI integrates directly with policy admin and CRM systems to enable this level of personalization at the point of call placement, not as a post-call data overlay.
The result is a renewal interaction that feels informed rather than automated - addressing the right policyholder, with the right information, at the right time.
Conversion rates from personalized outbound voice AI outreach consistently outperform human-agent generic reminder calls, particularly in Tier 2 and Tier 3 markets where in-language communication in the customer's preferred language is a decisive factor.
Claim status queries
A customer calling to check the status of a claim is anxious, often having already submitted documentation, and acutely sensitive to wait times and vague responses. A queue hold of even four minutes in this context erodes trust meaningfully.
Voice AI that integrates directly with claims management systems can resolve this category of call entirely. When a policyholder calls, the voice AI authenticates identity through policy number and mobile verification, queries the claims system for real-time case status, and delivers a specific, accurate update - "Your claim of Rs. 2,40,000 is currently in the medical review stage. The expected decision date is 18 May. You will receive an SMS confirmation once the decision is logged." - without a single second of hold time.
Haptik's claims query automation is built on real-time API integration with claims management platforms, ensuring that the information delivered is current and case-specific rather than a generic status message.
Policy detail requests
Policy information queries - "What is my sum assured?", "Is dental treatment covered?", "What is the waiting period for critical illness?" - are among the highest-volume inbound query types for any insurer, and among the safest to automate. The answers are contained in policy documents that are structured, version-controlled, and retrievable.
Voice AI handles this category by surfacing answers from policy document repositories in real-time, applying natural language understanding to match the customer's question to the relevant policy clause.
Haptik's platform supports document-grounded response generation, meaning the voice AI agent for insurance cites its answers from the actual policy terms rather than generating approximations. This matters for both accuracy and compliance.
Lapse and surrender prevention
Lapse and surrender calls are among the most commercially significant interactions an insurer can make.
A policyholder who calls to surrender a policy is signaling a decision that can often be reversed with the timely intervention:
- Clarification on surrender value implications
- Premium holiday option
- Policy restructuring discussion
Proactive voice AI outreach for at-risk policies - those with missed premium payment alerts, reduced payment activity, or surrender intent signals in CRM data - allows insurers to intervene before the call arrives inbound.
Haptik's outbound voice AI can be configured to trigger lapse prevention calls based on policy management system flags, opening a personalized conversation that explores the customer's concern before escalating to a human retention specialist where required.
KYC reminders and document collection nudges
KYC completion is a persistent operational bottleneck for insurers.
Incomplete KYC flags policies for regulatory risk and delays claim processing. Chasing document submissions through human agents is time-consuming and often ineffective because the volume of pending KYC cases far exceeds available outreach capacity.
Voice AI handles this cleanly - placing outbound calls to policyholders with pending KYC, explaining the specific document required, and in integrated deployments, sending a follow-up message with a direct upload link or guiding the customer to the nearest collection point.
New policy onboarding welcome calls
The first 90 days of a policy relationship are the highest-churn period in insurance. New policyholders who do not understand their coverage, do not know how to file a claim, or never receive a welcome interaction are significantly more likely to lapse than those who receive structured onboarding.
Voice AI welcome calls deliver a consistent onboarding experience - confirming policy details, explaining key benefits and exclusions in plain language, providing the claim intimation number, and answering initial queries - at the moment the policy is issued.
This early touch establishes the communication channel and reduces inbound query volume in subsequent weeks.
ALSO READ: Voice AI Use Cases for Customer Support That Actually Move the Needle
Compliance Is the Architecture
Do-not-disturb and calling window compliance
TRAI's DND regulations and IRDAI's fair practice guidelines define strict constraints on when and how insurers can contact policyholders.
Calling outside permitted windows or reaching numbers on DND registries exposes insurers to regulatory penalties and policyholder complaints.
Haptik's voice AI platform enforces these constraints at the infrastructure level. DND list validation is executed before every outbound dial. Calling windows are configured as hard system constraints, ensuring compliance is structural. It cannot be overridden by operational pressure to hit contact targets.
Consent recording and interaction audit trails
Every voice interaction executed through Haptik's platform generates a full audit trail - call timestamp, policy ID, interaction transcript, consent acknowledgment event, escalation trigger (if any), and outcome code.
These logs are stored in query-able format, enabling rapid retrieval for IRDAI inspection, internal audit, or grievance resolution.
Consent capture in Haptik's architecture is a structured interaction step - the customer must explicitly acknowledge the disclosure and consent statement before the interaction proceeds to a product discussion.
How voice AI handles the 'I want to speak to a human' moment
The escalation moment is the most important interaction design decision in insurance voice AI. Handled poorly, it creates frustration that erodes all the goodwill built in the preceding automated interaction. Handled well, it becomes a seamless handoff that increases rather than decreases customer satisfaction.
Haptik's voice AI platform manages escalation through a live agent handoff protocol that passes conversation context - what was discussed, what the customer requested, what the policy status is - to the receiving agent in real-time. The customer does not re-explain their situation. The agent begins with full context. This warm handoff architecture is one of the most consistent differentiators in Haptik's enterprise deployments.
Measuring Voice AI ROI in Insurance

ROI for voice AI in insurance is measurable across three primary vectors - renewal conversion, claim query containment, and agent load deflection. The infographic below captures benchmark performance from enterprise deployments:
Renewal conversion lift from proactive voice AI outreach
Enterprise deployments of outbound voice AI for renewal reminders consistently show conversion lift of 40-65% compared to uncontacted control groups - not because the AI is more persuasive, but because it contacts more policyholders, more reliably, at the right time.
Contact rate - the percentage of the eligible renewal universe actually reached - is the primary driver of renewal conversion, and voice AI dramatically expands this rate without adding headcount.
Claim query containment rate and handle time reduction
Claim status query containment rates - the percentage of inbound claim calls fully resolved without human agent involvement - typically reach 65-75% in deployments with deep claims management system integration.
For the 25-35% that require human escalation, the voice AI's pre-qualification and context capture reduces average handle time by 40-50%, because agents begin the call with authentication and case status already surfaced.
Agent load deflection
The most strategically important ROI metric is agent reallocation.
When voice AI absorbs 60-70% of inbound query volume, the agent workforce is freed to handle the interactions that genuinely require human judgment:
- Complex claim disputes
- Surrender prevention conversations
- High-value policy restructurings
- Customer escalations
This shift from reactive support handling to proactive retention work changes the profile from a cost center to a revenue protection function.
The Haptik Advantage: Enterprise Voice AI Built for Insurance
12+ years of AI deployment experience
Haptik has been building enterprise conversational AI infrastructure since 2013 - before large language models, before the current wave of voice AI investment, and before most insurers had begun evaluating the space.
This deployment history matters because insurance voice AI is a system that must be configured, tuned, and refined through real-world interaction data, compliance review cycles, and integration work with policy administration systems that predate modern API architectures.
500+ enterprise deployments across BFSI
Haptik's BFSI deployment portfolio spans life insurers, general insurers, health insurers, and lending institutions - giving the platform a breadth of insurance-specific interaction context that generic voice AI vendors cannot replicate.
The training data, conversation flows, and compliance configurations that power Haptik's insurance voice AI are informed by hundreds of real-world deployments, not sandbox evaluations.
No vendor lock-in, full integration flexibility
Haptik's voice AI platform is designed for integration. It connects to existing policy administration systems, CRM platforms, and claims management tools through standard APIs, without requiring insurers to migrate or replace core infrastructure.
RELATED: Integrating CRM, Service Desk, and Messaging Channels with AI Service Agent
This architecture protects technology investments already made and allows voice AI to augment the existing technology stack rather than compete with it.
Forward-deployed teams
Haptik's enterprise engagements are supported by forward-deployed implementation teams - conversation designers, integration engineers, and compliance architects who work within the insurer's environment rather than remotely.
This model accelerates deployment timelines, ensures conversation flows are validated against actual policyholder interaction patterns, and provides the compliance review support that insurance deployments require before go-live.
What to Ask from a Voice AI Partner in Insurance
Core insurance platform integration
A voice AI partner that cannot demonstrate live integration with at least one major policy administration system before contract signature is not production-ready for insurance.
Multilingual capability for Tier 2 and Tier 3 policyholder nases
India's insurance penetration growth is happening in Tier 2 and Tier 3 cities, where Hindi-only or English-only voice AI is a contact barrier.
ALSO READ: Voice Agents for Indian Languages: What Enterprise-Grade Really Means
Any voice AI deployment serving a pan-India policyholder base must support at minimum Hindi, Tamil, Telugu, Kannada, Bengali, and Marathi - with dialect sensitivity. Haptik supports 10+ Indian languages with the phonological and dialect-level accuracy required for insurance conversations in regional markets.
IRDAI-aligned interaction logging and consent management
Demand a vendor who can demonstrate - live, in a compliance review session - how their platform captures consent, logs interactions, validates DND compliance, and generates audit-ready exports.
If the compliance architecture requires manual configuration or is not auditable through the platform's own tooling, it is a risk that could surface at the wrong time.
FAQs
Yes - voice AI integrates with claims management systems in real-time, pulling live case data to give accurate, personalized updates without requiring human agents for status calls. The response reflects the current state of the specific claim.
At minimum: Hindi, Tamil, Telugu, Kannada, Bengali, and Marathi - aligned to policyholder geography. Haptik supports 10+ Indian languages with dialect sensitivity, enabling accurate, natural-sounding interactions across regional policyholder bases.





source on Google