Voice AI Agents for Healthcare: Reducing No-Shows, Improving Adherence and Patient Engagement
source on Google

Picture a 500-bed tertiary hospital in Pune on a busy morning. The OPD is running behind schedule - because four of the first twelve specialist slots are empty. The patients who booked them last week simply did not show up. The slot, the doctor's time, and the hospital's revenue evaporated quietly - the way they do, every single day, in thousands of facilities across India.
Every missed appointment costs a hospital between Rs 800 and Rs 3,000 in direct and indirect costs, and India's healthcare system absorbs millions of them every year. Layer on top of that the silent epidemic of medication non-adherence - where patients with chronic conditions skip doses, interrupt courses, or abandon treatment plans entirely - and you have a two-front operational and clinical crisis that traditional patient engagement methods are simply not built to solve.
Voice AI agent, deployed intelligently across the patient journey, addresses both problems at scale - without overburdening clinical or administrative staff.
This blog outlines where voice AI creates the most measurable impact in healthcare operations, and what enterprise-grade deployment looks like in practice.
The Patient Engagement Crisis Driving Healthcare Operational Costs
The cost of disengaged patients goes far beyond empty slots.
Across appointment management, medication adherence, and post-discharge follow-up, the operational and clinical consequences compound quickly - and the root cause is consistently the same: patients were not reached in time, through the right channel, in a language they understood.
No-show rates in Indian healthcare: The real numbers
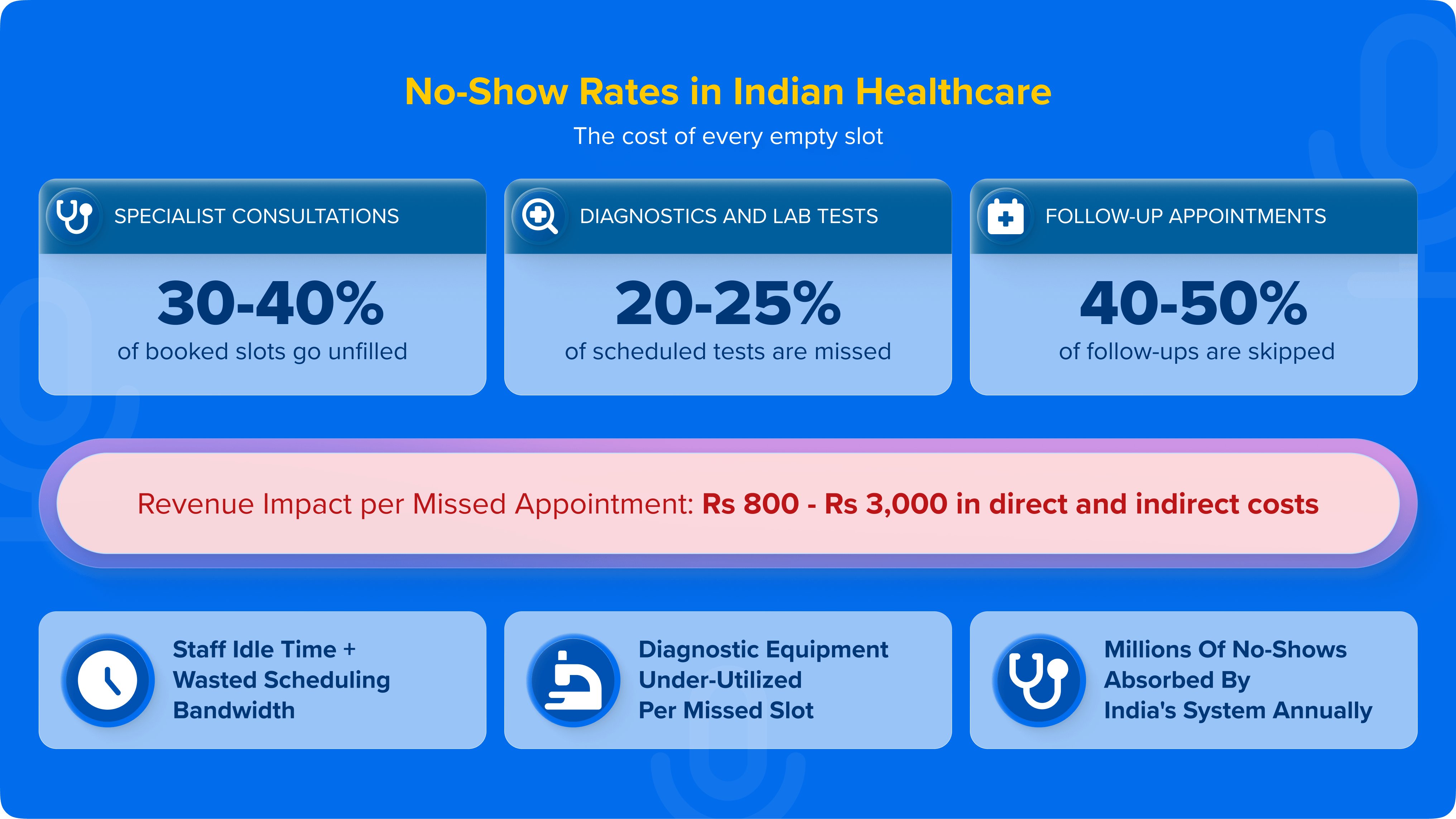
No-shows are a structural problem in Indian healthcare. Industry data and hospital operational benchmarks consistently point to the following:
In a 200-bed hospital running 400 OPD consultations daily, even a 20% no-show rate represents 80 missed appointments - translating to Rs 64,000 to Rs 2,40,000 in foregone revenue every single day. The aggregate, system-wide impact runs into billions of rupees annually. What makes this particularly frustrating for hospital operations teams is that a significant proportion of no-shows are preventable - patients forget, get confused about timing, or are simply not reached with a timely reminder.
Medication non-adherence: the silent driver of readmissions
If no-shows are the visible face of patient disengagement, medication non-adherence is its costly underbelly.
Across chronic condition management - diabetes, hypertension, cardiac care, oncology support - studies consistently show that 40-60% of patients do not take medications as prescribed. The downstream consequences are predictable and expensive: emergency readmissions, accelerated disease progression, avoidable hospitalization costs, and, for insurers and healthcare systems, spiralling claims.
For hospital operations heads and digital health product leaders, the data presents a clear mandate: patient engagement after discharge is not a courtesy service - it is a clinical and financial necessity.
The challenge is doing it at scale without proportionally scaling the workforce. This is precisely the gap that medication adherence automation through voice AI for healthcare is built to close.
Why phone-based patient engagement still outperforms app-based alternatives
Before any conversation about AI-powered engagement channels, it is worth confronting a persistent assumption in digital health: that smartphone apps are the future of patient communication.
For a narrow, urban, digitally native demographic, this may be partially true. For the majority of India's patient population - particularly in Tier 2 and Tier 3 markets, and across the 45-plus age bracket that accounts for the bulk of chronic condition management - it is demonstrably false.
App adoption in healthcare contexts remains low outside metro areas. Notification fatigue is high. Literacy barriers exist. And crucially, apps require patients to take an action - to open, to read, to respond. A voice call requires only that a phone rings.
Voice remains India's most universally accessible communication channel. Healthcare voice AI agents leverage this reality, delivering personalized reminders, confirmations, and follow-up calls in the patient's preferred language, at the right time, with the capacity to handle responses dynamically - without human agents on the line.
Where Voice AI for Healthcare Delivers Measurable Impact
Across the patient journey - from pre-appointment engagement to post-discharge monitoring - voice AI creates operational leverage at every touchpoint where traditional manual outreach struggles with scale, consistency, and cost.
Appointment reminders and confirmation calls
The most immediate ROI case for voice AI in healthcare is appointment reminder automation. Haptik's voice AI agents are deployed to initiate outbound reminder calls 48 and 24 hours before a scheduled appointment, confirm attendance, and dynamically handle responses - including rescheduling requests - within the same call flow.
Unlike messaging reminders (which patients increasingly ignore) or manual calls (which do not scale), voice AI reminder campaigns achieve confirmation rates of 75-85% on outbound calls - with zero agent involvement for routine confirmations.
The result is a measurable, near-immediate reduction in no-show rates, typically in the range of 18-35% within the first 90 days of deployment.
Rescheduling
When a patient cannot make their appointment, the follow-through process - cancellation capture, slot reassignment from a waitlist, and rebooking confirmation - typically requires multiple touchpoints and significant agent time.
Voice AI handles this end-to-end:
- Identifying available slots in real-time via appointment management system integration
- Offering the patient alternatives in the same call
-
Confirming the new booking without human intervention
Haptik's voice agents integrate directly with scheduling platforms, enabling live slot visibility and seamless rebooking flows - a capability that reduces the downstream administrative load on contact center teams.
Post-discharge follow-up calls
Post-discharge is where patient engagement most directly intersects with clinical outcomes.
Patients sent home after a procedure, surgery, or acute episode are statistically most vulnerable in the first 72 hours and first week - and most likely to be unreachable through traditional follow-up systems.
Voice AI enables structured post-discharge call programs at scale:
- Checking in on recovery
- Prompting symptom self-assessment (within defined, safe parameters)
- Verifying medication initiation
- Flagging high-risk indicators to a human care coordinator
Haptik's voice agents include configurable escalation triggers: if a patient reports specific symptoms, expresses distress, or meets defined risk criteria, the call is immediately transferred to a clinical staff member with full conversation context.
Medication adherence reminders
Medication adherence automation through voice AI for healthcare addresses the fundamental failure mode of most adherence interventions: they are generic, infrequent, and easy to ignore.
Haptik's voice agents deliver personalized, time-specific medication reminders calibrated to the patient's prescribed regimen - and can dynamically adapt based on responses, flagging missed doses or refill needs for follow-up.
For chronic disease management programs - diabetes clinics, cardiac rehabilitation, or oncology support - this represents a step-change in adherence infrastructure.
Enterprises deploying structured voice AI adherence campaigns have observed up to 30% improvement in self-reported adherence rates among enrolled patient cohorts.
Diagnostic report availability notifications
Patient anxiety around pending test results is a well-documented driver of unnecessary inbound calls and walk-ins.
Voice AI enables proactive, automated notification the moment a diagnostic report is available - with the option to direct the patient to a portal or schedule a consultation to review results with a physician.
ALSO READ: Voice Agents for Enterprises: How Inbound and Outbound Calling Works?
This single use case materially reduces inbound call volume for diagnostics and pathology labs, freeing front-desk and contact center capacity for higher-value interactions.
Preventive health screening campaigns
Beyond reactive patient management, voice AI for healthcare enables proactive population health outreach.
Hospitals and health systems can deploy outbound voice AI campaigns for preventive screenings - cancer checks, cardiovascular risk assessments, diabetic retinopathy screening, AND vaccination drives - reaching thousands of patients per day with personalized, contextually relevant messaging.
Haptik's AI voice agent supports campaign-level deployment with dynamic list management, call outcome tracking, and integration into CRM and patient management systems - giving operations teams full visibility into campaign performance in real time.
Patient satisfaction surveys via voice AI
CSAT and NPS measurement in healthcare has historically suffered from low response rates on paper forms and digital surveys. Voice AI dramatically improves survey completion rates by engaging patients in a brief, conversational post-encounter or post-discharge call.
Haptik's voice agents can administer structured satisfaction surveys, capture open-ended feedback through speech recognition, and surface insights to quality and operations teams.
For hospital CX heads and quality improvement teams, this creates a continuous, high-fidelity feedback loop that paper and app-based surveys simply cannot match.
Data Privacy and Compliance in Healthcare Voice AI
Deploying voice AI at enterprise scale in healthcare is not simply a technology decision - it is a data governance commitment. For hospital leadership and digital transformation teams evaluating voice AI vendors, compliance architecture is a non-negotiable filter.
RELATED: Data Privacy in Voice AI: The Enterprise Compliance Guide for 2026
DPDP Act compliance for patient health data in voice interactions
India's Digital Personal Data Protection (DPDP) Act 2023 establishes clear requirements for the collection, processing, and retention of personal data - including health-related data captured in voice interactions.
Haptik's platform is built with DPDP-aligned data handling as a foundational design principle: explicit consent capture at call initiation, purpose limitation in data use, and configurable retention and deletion policies that align with institutional data governance frameworks.
HIPAA-aligned architecture for global healthcare enterprises
For healthcare enterprises operating across geographies - or those working with international insurance and healthcare partners - HIPAA-aligned architecture is a baseline expectation.
Haptik's voice AI infrastructure supports HIPAA-compliant deployment configurations, including end-to-end encryption of voice data, role-based access controls, comprehensive audit trails, and Business Associate Agreement (BAA) readiness for relevant deployments.
When to escalate: Safeguards for high-risk patient interactions
No enterprise voice AI deployment in healthcare should be without a defined escalation framework. Haptik's platform includes multilayer safeguards: sentiment analysis to detect patient distress, keyword-triggered escalation protocols, and seamless warm transfer to human care coordinators - with the full conversation context transferred simultaneously.
The principle is clear and non-negotiable: voice AI handles administrative and routine engagement touchpoints autonomously. Any interaction that enters clinical, emotional, or risk territory is escalated to a qualified human. This boundary is not a limitation of the technology - it is a deliberate design choice that responsible healthcare AI vendors must enforce.
Multilingual Healthcare Voice AI
India's linguistic diversity is not a footnote in healthcare voice AI deployment - it is the primary design challenge. A voice AI that speaks only Hindi or English will reach a fraction of the patient population that most hospital networks serve.
Why medical conversations demand dialect-sensitive language models
Healthcare conversations are not simply translated. Medical terminology, dosage instructions, symptom descriptions, and scheduling contexts carry meaning that can shift significantly across dialects and regional variations. A voice AI built on generic multilingual models will introduce comprehension failures at precisely the moments where clarity matters most.
ALSO READ: Voice AI for Indian Languages: What Enterprise-Grade Really Means in 2026
Haptik's voice AI platform supports 10+ Indian languages with dialect-aware models specifically trained on healthcare conversation contexts. This goes beyond vocabulary - it encompasses natural conversation rhythm, culturally appropriate interaction patterns, and the ability to handle code-switching (mixing of languages) that is common in real patient calls.
Building for low-literacy patients: voice-first design principles
For patient segments with low health literacy or limited reading ability, voice is not simply a preferred channel - it is the only viable one. Voice-first design for these demographics requires specific principles: short sentences, plain vocabulary, confirmation-seeking at each step, and the avoidance of jargon entirely.
Haptik's conversational design framework includes low-literacy configuration modes, with simplified prompt structures and WhatsApp-based follow-up confirmation options for patients who prefer a text record of their interaction. This multi-channel close - voice engagement followed by a WhatsApp confirmation - has demonstrated measurably higher comprehension and follow-through rates in Tier 2 and Tier 3 deployments.
The Haptik Advantage - Healthcare Voice AI at Enterprise-Scale
The gap between a working voice AI demo and a production-grade healthcare deployment is significant. Enterprise healthcare environments demand integration depth, compliance architecture, and outcome accountability that most healthcare voice AI platforms are not built to deliver.
Integration with HIS, EMR, and appointment management platforms
Voice AI in healthcare is only as useful as its ability to read from and write to the systems that run hospital operations. Haptik's platform supports API-based integration with leading Hospital Information Systems (HIS), Electronic Medical Records (EMR) platforms, and appointment management systems - as well as custom-built systems through documented API frameworks.
RELATED: Integrating CRM, Service Desk, and Messaging Channels with AI Service Agent
This integration depth means that when a patient calls in or receives a reminder call, the voice agent has live access to their appointment data, preferred language settings, care program enrolment, and - where appropriate - relevant clinical context. It is the difference between a voice bot that reads a script and a voice AI that has a conversation.
Privacy-first architecture with on-premise deployment options
For healthcare enterprises with data residency requirements - government hospitals, large private health systems, institutions operating under specific regulatory constraints - cloud-only voice AI deployment may not be an option.
Haptik supports on-premise deployment configurations, giving CIOs and data governance teams full control over where patient data lives and how it is processed.
This is not a commonly offered option in the voice AI vendor landscape, and it is a meaningful differentiator for enterprise healthcare procurement teams evaluating long-term vendor risk.
Proven in high-volume healthcare deployments with outcome SLAs
Haptik's voice AI platform has been deployed in high-volume healthcare contact center environments, managing tens of thousands of patient interactions per day with documented outcomes against SLAs covering no-show reduction, confirmation rates, and CSAT improvement.
For hospital operations heads and digital health leads who need to justify voice AI investment to a leadership team, outcome SLA accountability is not a nice-to-have - it is the basis of the business case. Haptik engages with enterprise healthcare clients on defined success metrics from pre-deployment scoping, with measurement frameworks built into the deployment roadmap.
Metrics That Matter in Healthcare Voice AI
Evaluating the ROI of a voice AI deployment requires a clear measurement framework - not vanity metrics. The following represent the core KPIs that hospital operations and digital health teams should track from day one.
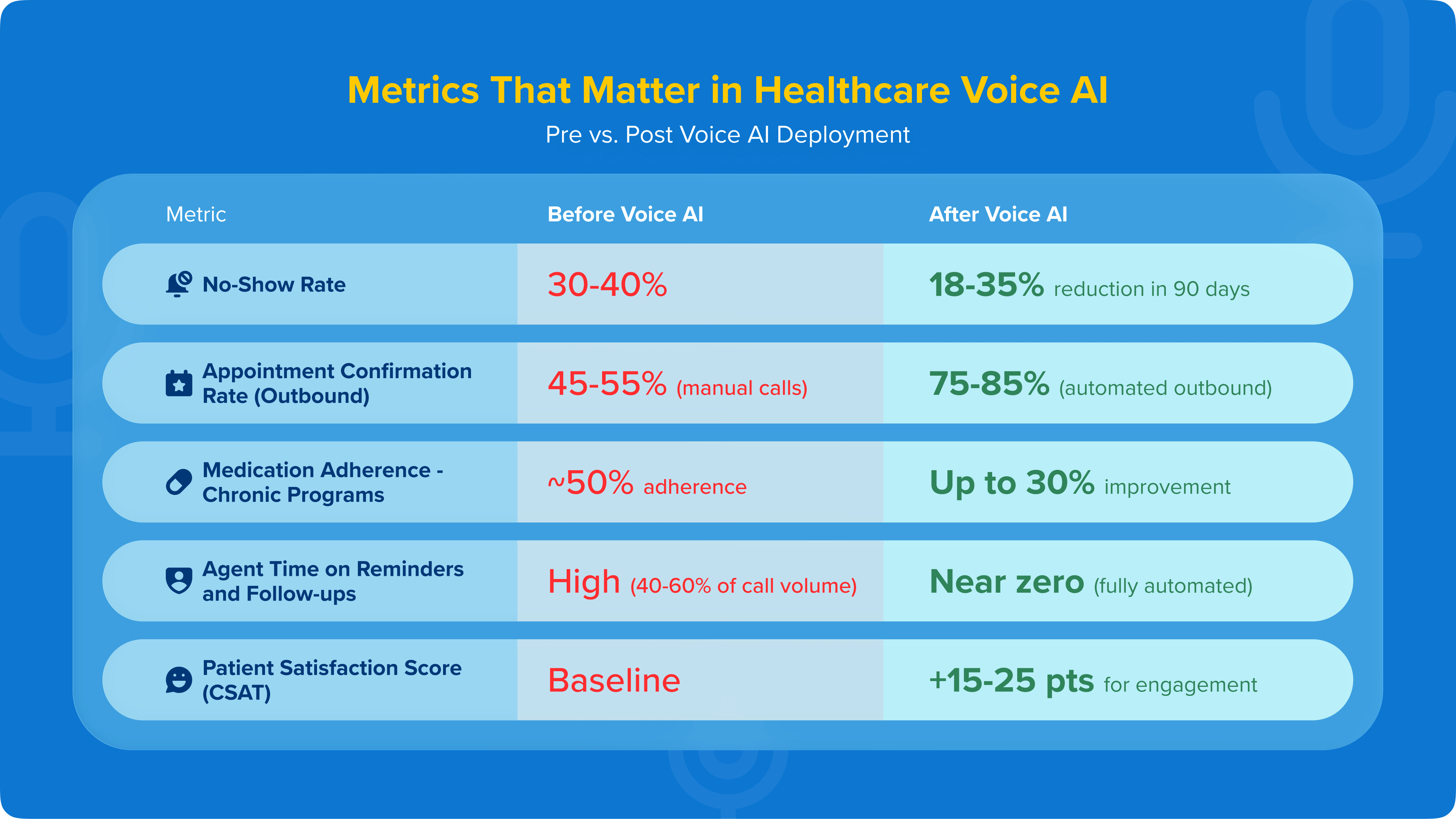
No-show rate reduction (pre vs. post voice AI deployment)
Baseline no-show rates by appointment type (specialist, diagnostic, follow-up) should be established in the 90 days before deployment and tracked weekly post-deployment.
Enterprises deploying structured voice AI reminder campaigns typically see 18-35% reduction in the first 90 days.
Appointment confirmation rate via automated outbound
The percentage of outbound reminder calls that result in a confirmed attendance, rescheduling request, or explicit cancellation - as opposed to no answer or no response.
A well-configured voice AI outbound campaign targeting 75-85% confirmation rate is a reasonable benchmark for mature deployments.
Medication adherence improvement rate
For chronic disease management programs, adherence improvement rate among enrolled patients (measured via self-report, refill rate proxy, or integration with pharmacy data) is the key clinical outcome metric.
A 20-30% improvement in adherence rates is the expected range for structured voice AI reminder and check-in programmes.
FAQs
For administrative touchpoints - reminders, scheduling, report notifications - yes. For clinical conversations covering symptoms, diagnoses, or treatment guidance, voice AI should route to a human clinician, always. Haptik's platform enforces this boundary through configurable escalation triggers that are defined and tested as part of the deployment process.
Leading platforms including Epic, Practo, Lybrate, and custom HIS systems. Integration is API-based and handled during deployment, with Haptik's implementation team working directly with hospital IT and operations teams to configure live data flows.





source on Google